|
With the holiday season approaching, many of us think about our waistlines and dieting. Some will start dieting before the holidays to fit into those party clothes. Others will contemplate strategies for eating during the holidays to minimize gain with the goal to lose those extra pounds after the holidays. You know, the proverbial “New Year’s Resolution.” All-in-all concerns about our weight create much angst during this joyous time of year. Here are the highlights from two presentations at the 2014 Academy of Veterinary Internal Medicine Symposium in Nashville, Tennessee, about weight loss strategies for cats: Chronic Calorie Reduction Chronic calorie reduction is a weight loss strategy based on restricting calories at a calculated level and maintaining or reducing that level of calories until a cat achieves its ideal weight. In this particular study, 32 client owned, obese cats were evaluated by a sophisticated X-ray technology (Dual-Energy X-ray Absorptiometry or DEXA) to determine their ideal body weights (IBW). The cats were then put on a diet that delivered 80% of the calories necessary for their resting energy requirement, or RER. RER is the absolute minimum number of calories necessary for body function at complete rest; not the amount of calories needed for maintenance energy requirement (MER) that includes normal, regular daily activities. The cats were fed this way until they reached their IBW, or until 104 weeks (2 years), whichever came first. Twenty-six percent of the cats left the study early due to owner non-compliance. Owner relocation, cat aggression to researchers, and other medical reasons caused another nine cats to drop from the study. Of the seventeen cats that finished the study, thirteen (76%) achieved their IBW within the first year. Three other cats achieved IBW in the second year, and one cat did not achieve IBW in the time period. Calorie adjustments during the testing period varied from as low as 40% of RER calories to as high as 100% of RER calories based on periodic weight monitoring. Periodic blood testing ensured the safety of the diet for the cats. Intermittent Calorie Restriction Intermittent calorie restriction is a weight loss strategy where animals are calorie restricted part of the time and fed normally the other times. In this study, 28 laboratory cats were divided into two equal groups. Fourteen cats were fed 75% of their estimated MER for six months. The other fourteen cats were fed 75% of their MER for the first two weeks of the month and then 100% of their MER for the second two weeks for twelve months. These cats were fed longer so that their calorie restricted period matched the period for the group that was chronically restricted for six months. Weekly body weights and monthly body scans for body fat were performed on all cats throughout the study period. The researchers found that the intermittent group lost more body fat than the chronically restricted group. They also found that 82% of the intermittent group achieved IBW in the time period versus only 36% of the chronic restriction group. A Peaceful Farewell provides compassionate in-home pet euthanasia to fellow pet owners in Chandler, Gilbert, Mesa, Tempe, Ahwatukee, Scottsdale, and most of the Greater Phoenix Metropolitan Area.
0 Comments
We’re familiar with the more common side effects associated with chemotherapy treatments: nausea, vomiting, lethargy, and hair loss. We all too easily relate to such signs, whether a result of our own personal experience, or those of friends/loved ones, or even through different media outlets. In veterinary oncology, every precaution is taken to limit such side effects. We accept a much lower rate of toxicity in dogs and cats, so our initial drug doses tend to be lower than our human counterparts. If side effects do occur, we are quick to reduce future dosages or delay treatments, keeping our patient’s safety at the forefront of concern. We want our patients to remain happy and healthy while enduring their protocols and to remain oblivious to the potentially negative repercussions of such serious remedies. There’s one side effect from chemotherapy that both veterinary and human oncologists remain persistently unable to adequately control. No matter how much effort we put in to preventing it, we are at the mercy of this most disturbing of adverse treatment-related injury. The concern we are speaking of is called financial toxicity. Financial toxicity, a term first coined by researchers in a study published in The Oncologist in 2013, describes how the “out-of-pocket expenses” of cancer treatment further drain the already stretched emotional and personal reserves of cancer patients, ultimately causing a significant decline in their overall quality of life and, in its most severe form, becoming an actual, palpable adverse side-event of treatment, leading to cessation of treatment. In the aforementioned study, researchers compared the results of surveys evaluating the impact of health care costs on well-being and treatment of cancer patients who contacted a national copayment assistance foundation with those from patients treated at an academic medical center. The results are staggering. Among 254 participants, 75% applied for drug copayment assistance. Forty-two percent of participants reported a significant or catastrophic subjective financial burden; 68% cut back on leisure activities, 46% reduced spending on food and clothing, and 46% used savings to defray out-of-pocket expenses. To save money, 20% took less than the prescribed amount of medication, 19% partially filled prescriptions, and 24% avoided filling prescriptions altogether. Copayment assistance applicants were more likely than non-applicants to employ at least one of these strategies to defray costs (98% vs. 78%). One conclusion from the study is that financial toxicity has both an objective side (a true enumeration of the burden the treatment places on the affected individual) as well as a subjective side (the less tangible distress the burden of treatment places on the patient). Another conclusion was that the consequences of financial toxicity reach far beyond the checkbook and extend into influencing important demographic information including response rates and survival statistics. Patients may actually stop taking medications, or even stop treatment entirely, because of the rising costs of their own healthcare and the burden this places on their lives. Not surprisingly, though financial toxicity isn’t typically discussed as an “actual” side effect in veterinary medicine, money plays a huge role in the oncological care for companion animals. Having worked directly in the trenches for so long, I would even venture that veterinarians deal with financial toxicity far more frequently than our human doctor counterparts. When cancer strikes a beloved pet, in addition to the emotional toll, the majority of owners must, at some point, consider the monetary impact of the diagnosis. Unlike humans diagnosed with cancer, our pets typically lack comprehensive healthcare to cover even routine costs, let along oncological care. A long-standing joke in veterinary medicine is to be wary of the owner who states “money isn’t an issue,” as most often it’s not an issue because they don’t have any. Cancer generally always imparts a sense of urgency, and I’ve witnessed many times where owners will make decisions regarding their pet’s care without full consideration of finances. In all seriousness, I have no way of knowing whether an owner who is giving me free reign to move forward with diagnostics and/or treatments is really able to afford things, or if they are making decisions based on emotions. I’ve seen many reactions to the cost of chemotherapy for pets. Most owners are well prepared by their primary care veterinarians for estimates of what different treatment plans could cost. There are definitely cases of complete “sticker shock,” where the numbers I discuss are not at all on par with what the owners were anticipating. Other times the reaction is the polar opposite, where there’s great surprise and the treatment is considered inexpensive. There’s not much I can do to control the cost of veterinary oncology care. Unfortunately, pricing schemes are complex; dictated by factors well beyond my professional “jurisdiction.” But it’s not enough for me to discuss only the physical signs associated with treatment when talking about side effects with owners. I’m equally responsible for attempting to prevent financial toxicity when I can. As is true for so many aspects of veterinary medicine (and life in general), clear communication is essential to ensuring everyone is on the same page. Your veterinarian should never judge you for deciding to put finances first when considering how to proceed with your pet’s care. And you should never judge your doctor for talking candidly about prices, estimates, costs, and expectations. I’ve been placed in that situation more times than I’d care to admit, and it’s unpleasant for all parties. We may not be able to eliminate financial toxicity from our treatment regimen, but veterinarians and owners both have a responsibility for making sure we pay close attention to even the subtlest signs of this important side effect. If we treat it as urgently and effectively as we do the more obvious signs, we’re guaranteed to reduce its impact and to further ensure that we maintain our patient’s quality of life, both in and out of the veterinary clinic. By Dr. Intile A Peaceful Farewell provides compassionate in-home pet euthanasia to fellow pet owners in Chandler, Gilbert, Mesa, Tempe, Ahwatukee, Scottsdale, and most of the Greater Phoenix Metropolitan Area.
One of the most common complaints veterinarian's get is how difficult it is for many cat owners to get their cat to the veterinarian (or anywhere else outside of the home, for that matter.) The chief reason these owners have difficulty is because their cat does not like the carrier and is often hard to actually get into the carrier. Being able to get your cat into and out of the carrier when needed is a necessity though. Cats need regular veterinary care and, in order to get to the veterinarian, a cat carrier is essential. There’s also the fact that, should an emergency occur that requires leaving your home quickly with your cat, being able to get your cat into the carrier quickly and easily without a struggle could mean the difference between life and death. Fortunately, there are some good ways to help your cat become acclimated to the carrier and to essentially make your cat’s carrier a retreat for him while he’s at home as well as making it a “home away from home”, a place where your cat feels safe and secure when out of your home. In other words, your cat’s carrier doesn’t have to be (and shouldn’t be) a scary thing for him. The American Association of Feline Practitioners (AAFP) have kindly provided the above infographic that contains some great tips for helping your cat become acclimated to the carrier. Definitely worth a look! Here are 6 TIPS:
It may take some time and patience but your cat can learn to love and enjoy his carrier. Once that happens, your life and your cat’s life will become much less complicated and stressful, especially when it comes time for that veterinary visit. A Peaceful Farewell provides compassionate in-home pet euthanasia to fellow pet owners in Chandler, Gilbert, Mesa, Tempe, Ahwatukee, Scottsdale, and most of the Greater Phoenix Metropolitan Area.
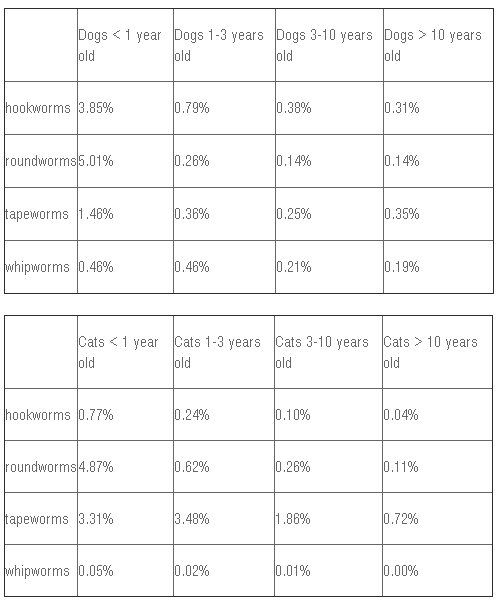
Why so many fecal exams? Because intestinal parasites are quite common in pet dogs and cats. Every year Banfield Pet Hospitals compiles a report based on the medical records of the patients they see. In 2013 they performed fecal examinations on 2,594,599 canine samples and 319,535 feline samples. Here are the percentage of tests that were positive broken down by age and type of parasite found. At first glance, these numbers may not look all that impressive, but digging a little deeper reveals a different story. Let’s look at the puppy and kitten numbers as examples since this is the age group most at risk for intestinal parasitism. What’s missing is the percentage of fecal samples that were positive for any type of intestinal parasite. Adding up the numbers in the columns above gives us a total of 10.78% for puppies and 9% for kittens. These percentages may not be exact since I’m sure some samples were positive for more than one type of parasite, but they give us a ball park figure.
However, a couple of issues suggest that these estimates are actually too low. First of all, whipworms are notoriously hard to diagnose via fecal exam. Their eggs don’t float very well in the most commonly used type of solution, and the worms release their eggs on an intermittent basis (in other words, the worms are present but their eggs are not). Secondly, while hookworms, roundworms, tapeworms, and whipworms are the “Big Four,” these tables say nothing about the incidence of Giardia, coccidia, and other types of intestinal parasites that can affect dogs and cats. The incidence of parasitism in pets is probably significantly higher than what the Banfield numbers show. In fact, a study published in 2009 looking at over a million canine fecal samples submitted to Antech Diagnostics revealed that 29.6% of those coming from dogs less than six months of age and were positive for intestinal parasites. Wow! So next time you head to the veterinary clinic, make sure you bring along a sample of your pet’s poop. You might be surprised at what’s hiding inside. Hippocrates said “Let food be thy medicine and medicine be thy food.” He knew that nutrition was the foundation for a healthy life. But more than that, he realized that it was substances in food that was key. What he didn’t know is how that key unlocked the power within the food we eat. Nutrigenomics has unlocked that mystery. This science will revolutionize dietary management for ourselves and our pets.
What is Nutrigenomics? We now know the entire human, canine and feline genetic code. We also have technological advances that allow us to look at the expression of genes to stimuli in real, nanosecond time. This means we can actually measure the effects of chemicals on the DNA of the cell. Neutrogenomics looks at these gene expression changes as a result of chemicals in foods. It identifies positive or negative responses to substances in foods. This information has verified some long standing beliefs in the benefits from certain foods and unmasked the failure of purported beliefs about other foods. Dog Food Example of Nutrigenomics Recently a well-known commercial producer of veterinary weight loss diets for dogs and cats introduced some new products. The company presented the results of they had achieved with these products at the latest Academy of Veterinary Internal Medicine Symposium that I recently attended in Nashville, Tennessee. They documented more fat loss and less muscle loss during weight loss using their proprietary diet blend. Fat loss is desirable during dieting. Muscle loss is not desirable because muscles are the leading source of caloric expenditure during dieting. But traditional weight loss diets involve muscle loss. This loss contributes to decreased calorie expenditure during dieting and contributes to the weight plateaus or even weight gain during the dieting process. The most effective weight loss diet would maximize fat loss while sparing muscle mass. And that was the aim of this company’s new diet formulation. Utilizing nurtigenomic analysis, their compelling results suggested that specific amounts of tomato pumice, coconut oil, and the amino acids L-lysine, L-carnitine and L-leucine triggered a favorable genetic change during a calorie restricted diet. The response of the cellular nucleus to the chemicals in these ingredients and these amino acids induced DNA to turn on genes that preferentially burned fat while preserving muscle. The data presented by the company is definitely limited and much more long term study is needed, but the power of this new science, nutrigenomics, is great stuff. This is especially true for those of us dedicated to homemade diets. Nutrogenomics and Homemade Pet Food At this point in time, most nutrigenomic information is proprietary and patented. The company above has made certain that their formula is protected. But this information will eventually become more readily available as the science becomes more common place. As it does, I will certainly incorporate these ingredients, in appropriate amounts, in my homemade diet programs so the power of nutrigenomics is available for your dog’s nutrition and greater health. For years, many have advocated for the inclusion of certain foods in our and our pet’s diets. With nutrigenomics we can now objectively analyze these claims and truly choose foods that in fact contain chemicals that can favorably alter our metabolism. This past September was designated as Happy Cat Month. That’s right — a whole month dedicated to keeping your cat happy and, of course, healthy.
Although we're now at the end of September, here are my top tips for keeping your cat happy throughout the year. Provide entertainment for your cat. Make sure your cat has lots of toys to play with and also make sure you set aside some personal time for interacting and playing with your cat. It will help you bond with your cat and also promote exercise, an important part of your cat’s routine to prevent weight gain and to keep your cat’s mind stimulated. Make sure all your cat’s needs are met by providing a clean litter box, perches, hiding places, and scratching surfaces. A clean food and water dish is essential as well. In multiple cat households, you’ll need additional sets of resources. Without these things, your cat is likely to become stressed and may start exhibiting unwanted behaviors. Stress can also be a contributing factor in illnesses for your cat. Keep your cat lean and fit. An overweight cat is more susceptible to a variety of diseases, including diabetes. Lots of toys and interactive play will be a big factor in increasing exercise for your cat, helping to burn calories and keep your cat at a proper weight. Diet, of course, plays a role as well. Feed your cat a high quality diet appropriate to your cat’s lifestage. Make sure the diet is complete and balanced. Feed in a proportion that keeps your cat from gaining excess weight. This next tip may not make your cat particularly happy but regular veterinary visits are essential for maintaining your cat’s health. Of course, a healthy cat is a happy one. Don’t forget about your cat’s teeth. Regular oral care will help keep your cat’s mouth healthy and help prevent dental disease, a common malady in cats. If your cat enjoys spending time outdoors, consider providing a catio. A catio is an outdoor enclosure that will confine your cat to a given space and provide protection from the threats faced by cats that spend time outdoors unsupervised. A catio can provide hours of entertainment for your cat. Another option is taking your cat outdoors on a collar or harness and leash. Your cat will enjoy investigating the outdoor environment and you will be there to keep him safe and secure. For more information about Happy Cat Month, more tips, information about adoption, and a list of helpful resources, please visit the CATalyst Council Happy Cat Month page. Is Your Cat Freaking Out?
Stress can make anyone a little crazy, even our cats. The tricky part is while the anxiety and fear associated with stress affects our cats in much the same way it does us, most cats tend to hide and mask their inner turmoil. Even worse, stress can be an indication your cat has a health issue. According to Patricia B. McConnell, Ph.D., a certified applied animal behaviorist, chronic stress even "suppresses the immune response, causing a broad range of illnesses." Here are some signs of stress you'll want to watch out for in your cat, especially if they occur suddenly. 1. Urinating Outside Litter Box It's annoying, smelly and a pain to clean up, but pay attention. Cats that urinate outside the litter box are trying to tell us something. Consult your veterinarian or a veterinary behaviorist to find out what it is. 2. Diarrhea, Constipation or other Digestive Issue This is another rather stinky situation and one that could be indicative of several things. Best not let it go and speak with your vet. 3. Excessive Grooming Cats are known for their fastidious grooming, but licking themselves raw or bald is a clear sign of distress. Skip the groomer and go straight for the vet's office. 4. Excessive Scratching Like compulsive licking, excessive scratching can be indicative of several health and behavioral issues. Make an appointment with your veterinarian before the problem gets out of hand. 5. Isolation Aloofness is second nature to cats. However, a cat should not be actively and constantly hiding from you and everyone else in the house. Once you've managed to wrangle him or her into a cat carrier, go to the vet. 6. Excessive Vocalization Many find the tone of a cat "talking" quite soothing, but be wary of unusually long or recurring bouts of panicked meows — especially if your cat is not the typical "talker." If it does happen, take your cat to the veterinarian rather than try to crack the kitty language code. 7. Decrease in Appetite Cats don't go on fasts or diets like we do so it's important to consult a veterinarian if your cat suddenly loses interest in food or stops eating altogether. 8. Increased Sleeping Just because cats can sleep up to 20 hours a day doesn't necessarily mean your cat will. By now you will have become accustomed to his or her sleeping schedule. Speak with your veterinarian if you're cat is sleeping more than usual or seems overly lethargic. 9. Aggression Towards Other Animals Fights or aggressive actions towards household pets or other animals can be a sign of a stressed or sick cat. Consult your veterinarian or a veterinary behaviorist before the problems gets worse. 10. Aggression Towards People A stressed or sick cat may also display aggression towards people, even you. Again, it's best to consult your veterinarian or a veterinary behaviorist immediately. Deciding whether to spay or neuter your pet is a big decision for a dog or cat owner. For many owners, the thought of anesthesia is scary. Some owners also worry that their pet’s personality will change after the surgery. Let’s talk about the benefits of spaying or neutering your pet and what you can do to ensure the health and well-being of your pet after the procedure.
In terms of the worries an owner faces at the prospect of spaying or neutering their pet, it’s important to note that, while it cannot be said there is no risk with anesthesia, the risk is minimal. Veterinarians today have anesthetic agents and monitoring equipment that make anesthesia safe and effective. And while behavioral changes can occur in spayed or neutered pets, the changes are more likely to be positive than negative. Spaying or neutering your pet is, undoubtedly, the socially responsible thing to do. By spaying or neutering your pet, you remove the potential for an accidental mating that will result in puppies or kittens that will add to the number of homeless pets currently found in shelters and rescues. But this is far from the only benefit. Benefits of Spaying a Female Pet A female pet that is spayed no longer comes in heat. As a result, there is no need to deal with the mess that female dogs can make when going through their heat cycle. Nor will you need to deal with the annoyance of a female cat in heat. For those of you unaware, dogs bleed while in heat. Cats, on the other hand, do not bleed but do vocalize, often in a quite disturbing manner. Both dogs and cats in heat will draw male dogs and cats, respectively, from far and wide. These animals can also make quite a nuisance of themselves as they hang around your home. There is also the fact that females that have been spayed, particularly those spayed at a young age, have a much lower risk of breast (or mammary) cancer. Many times, this form of cancer is malignant and can metastasize to the lungs, lymph nodes, and other parts of the body. However, spaying dogs and cats before their first heat cycle very rarely develop these tumors. Because the reproductive tract is removed during the spay procedure, female dogs and cats are no longer at risk for developing a severe and potentially fatal form of uterine infection known as a pyometra either. This is another major benefit. Benefits of Neutering a Male Pet Unaltered male pets often develop behavioral issues that can be difficult to tolerate and impossible to manage. They are more likely to roam and to fight with other animals, resulting in injuries that can be serious in nature. Intact males also tend to mark their territory more commonly than neutered males or females. In the case of an unaltered male cat, the urine has a very strong and pungent smell. These types of issues, though still possible in an unaltered male, are much less likely to occur. In addition, neutered males tend to be easier to train. Besides the behavioral benefits of neutering, there are some health benefits as well. Neutered males are less likely to develop prostate problems, including prostate cancer. Spayed/Neutered Pets Live Longer Than Those That Remain Intact For the vast majority of pets, spaying or neutering is the right decision. Overall, spayed and neutered pets live longer, healthier lives. However, there have been some studies that have indicated that dogs that are spayed or neutered, especially at a young age, may have a higher risk of certain forms of musculoskeletal and other disease, including bone cancer and cranial cruciate injuries. These studies generally have looked at a specific breed. This information makes it important to discuss with your veterinarian the best age at which to spay or neuter your pet. Your pet may have individual risk factors that influence the decision about when, or if, to spay or neuter. Responsibilities of a Pet Owner After a Pet Is Spayed/Neutered Spaying or neutering a pet does affect that pet’s metabolism. As a result, these pets may become more prone to weight gain if allowed to overeat. Choosing the correct diet and feeding the diet in quantities that keep your pet lean and fit are essential. Exercise is another important part of keeping your spayed or neutered pet lean and fit. Just as in people, exercise burns calories and keeps muscles and joints supple and healthy. All pets, whether spayed or neutered, should be visiting their veterinarian at a minimum once yearly for a thorough physical examination. Part of that physical examination will include an evaluation of your pet’s body condition, weight, diet, and exercise program. Your veterinarian can help you determine what diet, in what quantity, is appropriate for your pet as well as helping you develop an exercise program that will benefit your pet. Have you been following the news out of West Africa? The spread of the Ebola virus there is truly heartbreaking. While residents of the U.S. have little to fear from Ebola (unless you’re planning to travel to that part of the world), researchers here are still working hard to come up with new, potential therapies. You might be surprised to hear, however, that some of the most ground-breaking work is being done at the University of Pennsylvania’s veterinary school.
Dr. Ronald Harty is an associate professor of microbiology at Penn Vet, and in conjunction with other scientists from Penn Vet, the U.S. Army Medical Research Institute of Infectious Disease, Thomas Jefferson University, and Fox Chase Chemical Diversity Center, he is developing potential drugs that could revolutionize the way that Ebola and other viruses affecting people and animals are treated. I recently talked to Dr. Harty to learn more about his work. When asked why research into Ebola was being undertaken at a veterinary school, he replied: "I’m not a veterinarian, but I’m here at the vet school doing basic research working primarily on Ebola and other hemorrhagic fevers. But, we also do a lot of work on vesicular stomatitis virus (VSV) and rabies virus [both of which are significant animal pathogens]. VSV is actually a sort of distant cousin to Ebola. The makeup of the viruses — how they bud [exit the cell] and replicate, their genomes, the proteins they make — are very similar. VSV has served as a wonderful model system. It’s a virus we can fairly easily work with, using it as a surrogate to understand budding in the more pathogenic Ebola virus." One of the big problems in developing anti-viral drugs, particularly those that are useful against RNA viruses like Ebola, VSV, rabies, influenza, West Nile virus, human immunodeficiency virus (HIV), feline immunodeficiency virus (FIV), and feline leukemia virus (FELV), is that when these organisms replicate, they can mutate very rapidly and develop resistance to drugs. Dr. Harty explained that his team’s approach is innovative in that they are trying to develop drugs that are “host oriented.” "We are trying to target a virus-host interaction with our compounds. What we and others have found is that viruses like Ebola, rabies, and VSV hijack or recruit host proteins that help the virus to bud. The virus actually steals the function of these host proteins and uses it for its own purpose. We hypothesize that if we can target that virus-host interaction, we can block or slow down budding. We predict that the virus would not be able to mutate as readily to get around an inhibitor that is targeting, at least in part, a host function in comparison to one that just targets a specific viral protein. "The step that we are targeting is the very last step in budding, so the viruses are on the surface of the host cell. They can’t quite break free but are where the immune system can react to that pathogen. "[Budding] is analogous to having a car thief trying to speed away from a robbery. The drug would act like spike strips put down in front of that car; it would slow the infection down. We hope that will allow the immune system more time to develop a response, like the spike strips allow the police officer to catch up to the thief and arrest him. "The other really exciting part of the development of these compounds is they potentially have a very broad spectrum range of activity because many of these RNA viruses bud from cells using a similar mechanism. They all hijack the same host pathways. So what we and others have found is that if we can block budding of Ebola virus, for example, that same compound can block budding of other viruses like rabies, VSV, Marburg virus or even HIV. There is the potential to have a drug that could be effective against many different families of RNA viruses." Dr. Harty’s work reveals the deep connections between animal and human health. Hopefully, the compounds he and his team are developing eventually will benefit us all. Both the promises and perils of medical marijuana (MMJ) point to the need for science-based education, regulation and research. Many of us living in Colorado, one of the first states to legalize the sale of marijuana for both medical and recreational purposes, find ourselves touched deeply on a daily basis by stories that both uplift as well as cause grave concern for our veterinary patients.
On the up side, marijuana appears to afford a “lifesaving” alternative for a daunting gamut of difficult-to-treat disorders, including intractable epilepsy (seizure disorders that drugs cannot control). For companion animals, even the American Veterinary Medical Association website carries testimonials favoring veterinary cannabis, in which caregivers attest to significant benefits in their animals, who were unresponsive or intolerant of mainstream pharmaceuticals. Now that marijuana is becoming legal to buy for humans in a growing number of states, many are trying it on animals. But should you be administering it to your pet? Should your veterinarian? Unanswered QuestionsBecause of the higher toxicity of tetrahydrocannabinol (THC) in dogs compared to humans, many cannabis products sold for dogs list cannabidiol (CBD) instead of THC as the main active ingredient. (THC is the substance in cannabis that typically makes human users high.) Websites selling CBD-predominant substances for dogs may claim that their products are “completely safe” but lack reliable research to back those claims. There are, in fact, many potentially helpful chemicals in the cannabis plant, but THC and CBD usually outnumber the rest, although amounts are dependent on the strain of plant. What that means is that the ratio of cannabinoids (i.e., chemicals in the cannabis plant) differs among plants based on their genetics. While the CBD in cannabis does not make someone “high” in the usual sense, it may benefit human patients with various medical problems, including Crohn’s disease, post-traumatic stress disorder and multiple sclerosis. CBD reduces pain, inflammation and anxiety as well as seizure activity. Research suggests that CBD has lower toxicity and higher tolerability than THC in both humans and non-humans. However, research has not yet established safe dosing guidelines for either population, partly because of highly restrictive federal laws that prohibit scientists from thoroughly investigating its effects. A Deadly Uncertainty Lacking rigorous scientific evidence, veterinarians cannot determine safe dosages and THC/CBD ratios of medical marijuana for dogs, cats and other animals. Veterinarians and owners are left relying on anecdotal reports, trial and error and companies’ claims. If the tolerable and safe dose, whatever that might be, is exceeded, an animal may land in the local veterinary emergency clinic, and there are no antidotes for THC poisoning. While many insist that marijuana overdoses cannot kill, the consequences of cannabis can indeed turn deadly in dogs as the result of THC overdose. Dogs are most commonly exposed to cannabis through THC-laced edibles they find in the trash or in other opportune places, though some may ingest marijuana through purposeful exposure by their owners to tinctures, vapors and even homemade dog biscuits. The incidence of both intentional and unintended exposure is increasing as legalization spreads throughout the United States. As a cautionary tale, veterinary hospitals in Colorado have witnessed growing numbers of animals admitted for marijuana poisoning. Even before laws passed in Colorado allowing sales for recreational purposes, the number of dogs presenting with marijuana toxicosis quadrupled. Contributing factors beyond increased availability likely include a higher awareness among clinicians of the signs of poisoning, population shifts (e.g., marijuana “tourism” and immigration) and a greater willingness of clients to seek veterinary assistance for the condition. Depending on the dose and route of administration, problems usually appear within 30 to 60 minutes after exposure. The ASPCA’s Pet Poison Helpline lists 12 common signs of toxicity ranging from coma to seizures and respiratory depression to hyperactivity. Calls for Caution Much more needs to be done to make marijuana safe not only for pets but for humans, too. To both pets and people, marijuana-laced foodstuffs are indistinguishable from their innocuous counterparts, raising the risk of accidental ingestion by children, animals and unsuspecting adults. The amount of THC cooked into the cookies, chocolates and other foods can also take those intentionally consuming the products by surprise. For example, shortly after consuming a marijuana cookie, a college student jumped to his death from a motel balcony. In another case, a Denver man shot and killed his wife after supposedly eating cannabis candy. Those incidents underscore the urgent need for education, regulation and research. Unfortunately, federal restrictions on marijuana research have hampered investigation into both its value and dangers. Decade after decade, advocates of less restrictive marijuana laws have unsuccessfully petitioned the Drug Enforcement Administration (DEA) to rethink the listing of marijuana as a Schedule I addictive drug with no therapeutic value. Delisting cannabis would ease research restrictions and allow studies on safety and efficacy to move forward. Today, inadequate oversight of the amount of THC that producers are putting into each serving of edible marijuana is resulting in injuries, as is the lack of guidelines for and availability of testing, labeling and protective packaging. Consumers are confused about how much to eat and whether one batch of cookies or candies will produce the same effects as the next, turning self-medicating into a game of wild guessing. Safety Requires Study As a result, Colorado is earning the reputation as the Wild West of medical marijuana. Tying the hands of researchers and clinicians who desperately want to begin research is federal law that bars them from studying the safety and effectiveness of medical marijuana. That is putting the safety of people, pets and the public in jeopardy. The cure? Remove restrictions on research so that scientists, physicians and veterinarians can study cannabis carefully and without risking their licenses, federal funding and/or freedom through imprisonment. Only then will we be able to safely determine the benefits and appropriate uses of medical marijuana for veterinary patients. |
The PAW Blog...
For the LOVE of Pets The goal of this blog is to help educate pet owners by sharing pet health facts and pet news articles...and ... sometimes put a smile on your face with a cute or funny pet story! Categories
All
Archives
April 2024
Search for any topic...
|


 RSS Feed
RSS Feed

