Parvovirus Can Kill Your Puppy in 48 to 72 Hours, But Promising Treatment Is 90% Successful12/14/2014 About 10 years ago, before there was a name for West Nile virus, the mysterious disease was killing large populations of geese in South Dakota. Searching for an effective remedy, a group of researchers at the University of North Dakota discovered that antibodies contained in the yolks of goose eggs could be purified and given to birds with the virus, curing them. Soon afterwards, a company called Avianax was formed to test the treatment beyond geese. It turned out the goose antibodies had a beneficial effect against other diseases as well, including rabies, dengue fever, avian flu, and certain cancers. Avianax decided to focus first on using the antibodies against parvovirus in puppies, and initial trials of the company's parvoONE treatment (about 50 puppies in 7 states) resulted in an astonishing cure rate of 90 percent in as little as two days. Parvovirus Is Hard to Control and Costly to Treat Canine parvovirus is difficult to control -- especially in a shelter environment -- and expensive to treat. The virus is spread through animal waste and direct dog-to-dog contact. It is highly contagious and can live on surfaces for months. Some puppies die from the virus and others are euthanized because the antibiotics and other drugs needed to treat it can be too expensive – from $500 to $2,000 -- and take about a week to work. Parvo causes similar symptoms in all infected puppies and dogs, including vomiting, severe and often bloody diarrhea, lethargy, fever, and loss of appetite. In dogs infected with the virus, dehydration is a constant concern and can occur very quickly as a result of the vomiting and diarrhea. This is especially dangerous in very young puppies. Most deaths from parvo occur within 48 to 72 hours after the onset of symptoms, which is why immediate treatment is crucial for survival. Affordable Cure to Parvovirus Could Be Available in Spring 2015 The USDA issued a conditional permit to Avianax for parvoONE field trials that took place through November in Missouri, North Dakota, Minnesota, Iowa, Texas, North Carolina, and Arizona. Avianax chief operating officer Richard Glynn hopes to start selling the parvoONE antibody-based treatment for $75 a dose by next spring. "We went from being goose herders from South Dakota to an antibody company," Glynn said. "And we're not done yet." Vaccinating Your Dog Against Parvo Obviously, it's best to treat a parvovirus infection by preventing it from happening in the first place. Providing baseline protection (two correctly timed puppy vaccines) against the virus will in most cases provide your pet with lifetime immunity. Ideally, knowing when maternal antibody wears off in puppies allows for a perfectly timed immunization protocol. Dr. Ron Schultz has found that measuring titers in pregnant females allows vets to pinpoint exactly when the first vaccine will yield the best immunologic response in puppies. If this isn't possible, then the protocol I follow is to give a parvo/distemper shot before 11 weeks of age (9 weeks is ideal), and a booster at about 14 weeks. Two to four weeks after the second shot I titer to insure the puppy is successfully immunized against those diseases. This is a core vaccine protocol that provides the minimum number of vaccines to protect against life-threatening illnesses, without over-vaccinating. Remember, vaccinating before maternal antibodies wear off will be ineffective at protecting the puppy against disease. Keep in mind that it takes 10 to 14 days after the vaccination for adequate protection to occur. So when puppies are very young (and not immunized), it's important to keep them away from potential sources of the virus (no visits to the woods, dog parks, or shelters). Also, a small percentage of dogs will be non-responders, probably including the Great Dane puppy Sasha in the video above, who had three vaccinations against parvo and still contracted the virus. This means they will not develop immunity and will be susceptible to parvo all their lives. This is important information for dog owners to have, which is another reason I titer after the second round of shots. A Peaceful Farewell provides compassionate in-home pet euthanasia to fellow pet owners in Chandler, Gilbert, Mesa, Tempe, Ahwatukee, Scottsdale, and most of the Greater Phoenix Metropolitan Area.
1 Comment
 Hearing the news that your pet has been diagnosed with cancer can be both devastating and terrifying at the same time. It is natural to have many questions about exactly what the diagnosis means, what might happen to your pet as the cancer progresses, and what options you have for treating the disease. One of the most common questions owners ask veterinarians when their pet is diagnosed with cancer is "What caused my pet’s cancer?" Unfortunately, this is a very difficult question to answer accurately, as in nearly all cases cancer is typically caused by a combination of genetic and environmental influences, many of which may have occurred years before the diagnosis was made. The fact that certain types of cancers occur more often in particular breeds of dogs and cats lends much evidence to the concept of a genetic cause for the disease. We do know that the genetic mutations that cause cancer can occur in the reproductive cells of male and female animals, and these mutations can be passed on to puppies and kittens, giving rise to a heritable predisposition to different types of tumors. Most cancers, however, arise from mutations that occur to genes during a dog’s or cat’s lifetime that were not present at birth. These mutations can result from internal factors, such as exposure to naturally occurring hormones, or external factors, such as environmental tobacco smoke, chemicals, or even sunlight. In people we know that up to one-third of all tumors are related to environmental and lifestyle factors. In veterinary oncology, we have discovered that nutrition, hormones, viruses, and carcinogens such as smoke, pesticides, UV light, asbestos, waste incinerators, polluted sites, radioactive waste, and canned cat foods can increase the risk of cancer in pets. Some examples of known causes of cancer in companion animals include: Increased risk of mammary cancer in un-spayed female dogs and cats.
Studies have shown conflicting information regarding the risk of exposure to herbicides and/or pesticides and the development of cancer in pets. For example, some studies have shown an increased risk for the development of lymphoma, which is a cancer of white blood cells, while other studies have refuted the risk. Because the results are inconclusive its is generally recommend that owners should strive to minimize their pets’ exposure to these chemicals and discuss any concerns they may have with their primary care veterinarian. It is important to remember that it is often difficult to prove "cause and effect" when it comes to cancer. This is true for even well designed research studies designed to look at those exact parameters, so one has to be careful when researching this topic and not over interpret the available information. There are so many potential interactions between genes and environment influences that could lead to the development of a tumor, and ultimately, we may never be able to know exactly what caused the cancer in the first place. A Peaceful Farewell provides compassionate in-home pet euthanasia to fellow pet owners in Chandler, Gilbert, Mesa, Tempe, Ahwatukee, Scottsdale, and most of the Greater Phoenix Metropolitan Area.
Holiday Hazards Winter holidays are a wonderful time to enjoy family and friends. But with all the extra hustle and bustle you may forget to abide by the same pet-proofing measures you follow the rest of the year. We spoke with Dr. Justine Lee, Associate Director of the Pet Poison Helpline and Specialist at Animal Emergency & Referral Center of Minnesota, to discuss 10 common winter holiday hazards she and her colleagues encounter. Some of the items may surprise you. 1. Chocolate As tasty as chocolate can be for us, it can be plenty dangerous for our pets. Worse yet, there are many seemingly innocuous forms of chocolate pets can get into during the holidays — chocolate coins, baking chocolate morsels, even chocolate-covered espresso beans and macadamia nuts can dispense an unhealthy dose of methylxanthines to pets. Cats, it's important to note, can also be adversely affected if they ingest chocolate. But Dr. Lee points out that it's just that most cats have no interest in it. In fact, over 90 percent of chocolate toxicity calls to the Pet Poison Helpline are for dogs. 2. Alcohol Now it's highly unlikely any of your household guests would dare to give Fido or Fluffy a sip of their alcoholic drink, but they may not think twice about a piece of rum cake. Pets may also inadvertently become poisoned if they eat any unbaked bread dough. Once ingested, Dr. Lee Says, "the stomach acts as an artificial oven that basically metabolizes the yeast [from the unbaked dough] into ethanol and carbon dioxide." This can then cause the animal to bloat from the excess carbon dioxide and suffer from alcohol poisoning from the ethanol. 3. Grapes (and Raisins) Grapes and their dried cousins, raisins, are other common hazards for pets during the holidays. It may sound unusual, but any candied raisins found in fruit cake or grapes found on appetizer platters could spell bad news for your pet. "The other reason we get a lot of [grape and raisin poison] calls, Dr. Lee says, "is because holidays are a time when family [and friends] visit — and they are sometimes unaware that grapes and raisins are poisonous to dogs and cats." 4. Medications You may be stickler when it comes to pet-proofing your house, but once the holiday guests arrive that all goes out the window. Traveling household guests often leave open suitcases on the ground, where pets can easily get into prescription medications found Zip-loc bags. Suddenly you have a pet that can get into 20 different medications all at once. 5. Tinsel Anyone who has a cat needs to really watch out for when using this shiny object around the house, Dr. Lee says. In fact, you may be better off forgoing using tinsel on trees, wreaths, or garland this year. Tinsel is thin and sharp and can easily wrap itself around the intestines or ball up in the stomach once ingested. 6. Xylitol It may sound like some exotic instrument, but xylitol is just a sugar substitute found in some sugar-free candies, gum and recipes. When ingested by pets, xylitol may cause vomiting, loss of coordination, seizures, and in severe cases, liver failure. Don't let your sweet tooth accidentally become hazardous to your pet's health. 7. Plants Winter holidays wouldn't be the same without mistletoe and holly. Unfortunately, these are also two of the more toxic holiday plants to pets, causing severe gastrointestinal disorders, breathing difficulty, even heart failure in extreme cases. The dangers of poinsettias, on the other hand, are overhyped in Dr. Lee's opinion. Of course, while they are not safe for your pet, often the worse that happens to a dog or cat that ingests a small portion of the poinsettia is a bit of mild indigestion. 8. Liquid Potpourri Much like "regular" potpourri, liquid potpourri can freshen up any room. However this concentrated fragrance, which is typically simmered in a pot and then placed in a bottle for later use, can cause severe damage to your pet if ingested. "Cats," Dr. Lee says, "are super curious about [simmering] potpourri and drink the liquid, which then poisons them." Liquid potpourri also contains a cationic detergent, which is corrosive and can cause burns on a pet's tongue, difficulty breathing, and even excess liver enzymes. 9. Holiday Ornaments Although not poisonous, many ornaments have sharp edges that can cause perforations and lacerations to pets that try to chew on the decorations. We wouldn't dare ask you to strip the house of all the joy holiday ornaments can bring, but please safeguard them for the sake of your pet. 10. Electrical Cords Winter holidays bring with them plenty of connected devices —lights, lights, and more lights — along with the electrical cords and outlets needed to power these devices. Curious puppies and kittens are especially intrigued by the exposed wiring, Dr. Lee says, and are therefore most in danger of the burns or fluid accumulation in the lungs associated with electrical shocks. Take care where you place electrical cords and outlets, and when possible, place them out of reach from your pets. Be Prepared As you can see, the dangers for your pets are numerous. But with a little common sense and a lot of preparation you can minimize the danger. One of the most important aspects of being prepared is knowing what to do if an emergency should occur. Dr. Lee has some advice for that as well. "I always tell people to preprogram the contact numbers for your vet, nearest emergency hospital and the Pet Poison Helpline (855) 213-6680." So, what are you waiting for? Do it now! A Peaceful Farewell provides compassionate in-home pet euthanasia to fellow pet owners in Chandler, Gilbert, Mesa, Tempe, Ahwatukee, Scottsdale, and most of the Greater Phoenix Metropolitan Area.
Humankind has been searching for a “fountain of youth” for thousands of years. For dog owners, the perfect find wouldn’t just extend our lives but also those of our beloved canine companions. For years veterinarians have advocated a few strategies to potentially extend the lifespan of dogs including a 25% reduction in caloric intake and perhaps giving older dogs L-deprenyl. However, research supporting the use of L-deprenyl for this purpose is hardly definitive. Two scientists from the University of Washington are looking to expand our understanding of how dogs age and whether or not a different drug, rapamycin, might help them age better and live longer. The first part of the Dog Aging Project consists of a “Longitudinal Study of Aging in Pet Dogs,” the goal of which is to “perform the first nationwide, large-scale longitudinal study of aging in pet dogs, where individual animals will be followed throughout life to understand the biological and environmental factors that determine why some dogs die early or succumb to diseases such as cancer, kidney failure, and dementia, while others live to a relatively old age free from these problems.” The project’s second goal is “an intervention trial to treat middle-aged dogs with the FDA approved drug rapamycin. At high doses, rapamycin is used successfully in human patients to prevent organ transplant rejection and to fight cancer. At low doses, rapamycin slows aging and extends lifespan in several organisms, including mice, with few or no side effects.” The first phase of this study will enroll middle-aged dogs (6-9 years depending on breed) in a short-term (3-6 month), low-dose rapamycin regimen and follow age-related parameters such as heart function, immune function, activity, body weight, and cognitive measures. These animals will then be followed throughout life to determine whether there are significant improvements in healthy aging and lifespan. The next phase of the study will enroll a second cohort of middle-aged dogs into a longer-term, low-dose rapamycin regimen designed to optimize lifespan extension. As with phase one, several age-related parameters will be assessed before, during, and after the treatment period. Based on the mouse studies performed at the University of Washington and elsewhere, we anticipate that rapamycin could increase healthy lifespan of middle-aged dogs by 2-5 years or more. Rapamycin is off patent, which means drug companies aren’t interested in funding additional research into its potential use as an “anti-aging” treatment. This is why your help is needed. The Dog Aging Project is looking for donations to help with funding as well as canine “citizen scientists” to participate in the longitudinal study and the first phase of the interventional trial. Take a look at the project’s website for more information. A Peaceful Farewell provides compassionate in-home pet euthanasia to fellow pet owners in Chandler, Gilbert, Mesa, Tempe, Ahwatukee, Scottsdale, and most of the Greater Phoenix Metropolitan Area.
We’re familiar with the more common side effects associated with chemotherapy treatments: nausea, vomiting, lethargy, and hair loss. We all too easily relate to such signs, whether a result of our own personal experience, or those of friends/loved ones, or even through different media outlets. In veterinary oncology, every precaution is taken to limit such side effects. We accept a much lower rate of toxicity in dogs and cats, so our initial drug doses tend to be lower than our human counterparts. If side effects do occur, we are quick to reduce future dosages or delay treatments, keeping our patient’s safety at the forefront of concern. We want our patients to remain happy and healthy while enduring their protocols and to remain oblivious to the potentially negative repercussions of such serious remedies. There’s one side effect from chemotherapy that both veterinary and human oncologists remain persistently unable to adequately control. No matter how much effort we put in to preventing it, we are at the mercy of this most disturbing of adverse treatment-related injury. The concern we are speaking of is called financial toxicity. Financial toxicity, a term first coined by researchers in a study published in The Oncologist in 2013, describes how the “out-of-pocket expenses” of cancer treatment further drain the already stretched emotional and personal reserves of cancer patients, ultimately causing a significant decline in their overall quality of life and, in its most severe form, becoming an actual, palpable adverse side-event of treatment, leading to cessation of treatment. In the aforementioned study, researchers compared the results of surveys evaluating the impact of health care costs on well-being and treatment of cancer patients who contacted a national copayment assistance foundation with those from patients treated at an academic medical center. The results are staggering. Among 254 participants, 75% applied for drug copayment assistance. Forty-two percent of participants reported a significant or catastrophic subjective financial burden; 68% cut back on leisure activities, 46% reduced spending on food and clothing, and 46% used savings to defray out-of-pocket expenses. To save money, 20% took less than the prescribed amount of medication, 19% partially filled prescriptions, and 24% avoided filling prescriptions altogether. Copayment assistance applicants were more likely than non-applicants to employ at least one of these strategies to defray costs (98% vs. 78%). One conclusion from the study is that financial toxicity has both an objective side (a true enumeration of the burden the treatment places on the affected individual) as well as a subjective side (the less tangible distress the burden of treatment places on the patient). Another conclusion was that the consequences of financial toxicity reach far beyond the checkbook and extend into influencing important demographic information including response rates and survival statistics. Patients may actually stop taking medications, or even stop treatment entirely, because of the rising costs of their own healthcare and the burden this places on their lives. Not surprisingly, though financial toxicity isn’t typically discussed as an “actual” side effect in veterinary medicine, money plays a huge role in the oncological care for companion animals. Having worked directly in the trenches for so long, I would even venture that veterinarians deal with financial toxicity far more frequently than our human doctor counterparts. When cancer strikes a beloved pet, in addition to the emotional toll, the majority of owners must, at some point, consider the monetary impact of the diagnosis. Unlike humans diagnosed with cancer, our pets typically lack comprehensive healthcare to cover even routine costs, let along oncological care. A long-standing joke in veterinary medicine is to be wary of the owner who states “money isn’t an issue,” as most often it’s not an issue because they don’t have any. Cancer generally always imparts a sense of urgency, and I’ve witnessed many times where owners will make decisions regarding their pet’s care without full consideration of finances. In all seriousness, I have no way of knowing whether an owner who is giving me free reign to move forward with diagnostics and/or treatments is really able to afford things, or if they are making decisions based on emotions. I’ve seen many reactions to the cost of chemotherapy for pets. Most owners are well prepared by their primary care veterinarians for estimates of what different treatment plans could cost. There are definitely cases of complete “sticker shock,” where the numbers I discuss are not at all on par with what the owners were anticipating. Other times the reaction is the polar opposite, where there’s great surprise and the treatment is considered inexpensive. There’s not much I can do to control the cost of veterinary oncology care. Unfortunately, pricing schemes are complex; dictated by factors well beyond my professional “jurisdiction.” But it’s not enough for me to discuss only the physical signs associated with treatment when talking about side effects with owners. I’m equally responsible for attempting to prevent financial toxicity when I can. As is true for so many aspects of veterinary medicine (and life in general), clear communication is essential to ensuring everyone is on the same page. Your veterinarian should never judge you for deciding to put finances first when considering how to proceed with your pet’s care. And you should never judge your doctor for talking candidly about prices, estimates, costs, and expectations. I’ve been placed in that situation more times than I’d care to admit, and it’s unpleasant for all parties. We may not be able to eliminate financial toxicity from our treatment regimen, but veterinarians and owners both have a responsibility for making sure we pay close attention to even the subtlest signs of this important side effect. If we treat it as urgently and effectively as we do the more obvious signs, we’re guaranteed to reduce its impact and to further ensure that we maintain our patient’s quality of life, both in and out of the veterinary clinic. By Dr. Intile A Peaceful Farewell provides compassionate in-home pet euthanasia to fellow pet owners in Chandler, Gilbert, Mesa, Tempe, Ahwatukee, Scottsdale, and most of the Greater Phoenix Metropolitan Area.
It is amazing how little time is required for petting to make a big difference in their stress levels. At the 2014 American College of Veterinary Internal Medicine Symposium researchers presented an abstract synopsis of a yet to be published study of 15-minute petting sessions with shelter dogs. The results are illuminating and really reinforce the impact of companionship in helping shelter dogs adjust to potential adoption. The Dog Stress Study Fifty-five shelter dogs were subjected to one 15-minute petting session with an unfamiliar volunteer at a county animal shelter. The sessions were videotaped and the volunteers were given specific instructions on how to interact and pet the subject dogs. Saliva was collected from the dogs to analyze their body cortisol, or stress hormone, levels before and after petting. The heart rate of the dogs was also monitored for the entire 15-minute session. As expected there was a great deal of variation of response depending on the age, temperament, coping styles, and time spent in the shelter among the animals. In fact, cortisol levels before and after petting were not different. This suggests that stress was still a constant despite the petting session. Another explanation is that 15 minutes is a relatively short period of time to detect significant changes in body cortisol levels in saliva and would not reflect potential real changes in cortisol secretion. What was observed was a statistically significant decrease in heart rate and behavior changes consistent with a positive state of relaxation. The observation of the researchers is that “yes, 15 minutes does make a difference” for many shelter dogs. The Implications of the Dog Stress Study If only 15 minutes can make a difference, what difference could multiple 15-minute sessions make in the re-socialization of abandoned or lost pets? A Peaceful Farewell...Providing compassionate in home pet euthanasia to fellow pet owners in Chandler, Gilbert, Mesa, Tempe, Ahwatukee, Scottsdale, and most of the Greater Phoenix Metropolitan Area.
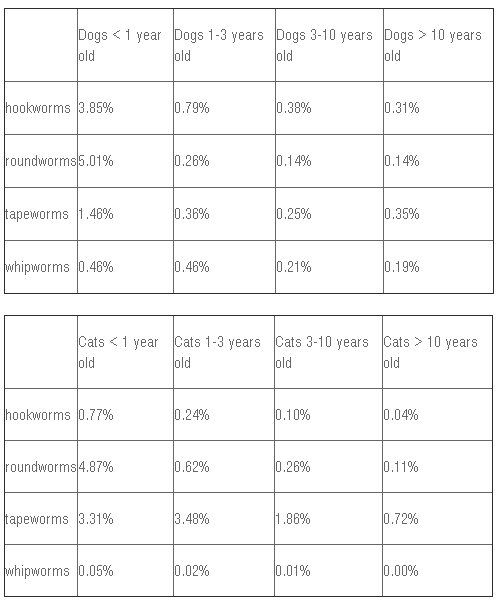
Why so many fecal exams? Because intestinal parasites are quite common in pet dogs and cats. Every year Banfield Pet Hospitals compiles a report based on the medical records of the patients they see. In 2013 they performed fecal examinations on 2,594,599 canine samples and 319,535 feline samples. Here are the percentage of tests that were positive broken down by age and type of parasite found. At first glance, these numbers may not look all that impressive, but digging a little deeper reveals a different story. Let’s look at the puppy and kitten numbers as examples since this is the age group most at risk for intestinal parasitism. What’s missing is the percentage of fecal samples that were positive for any type of intestinal parasite. Adding up the numbers in the columns above gives us a total of 10.78% for puppies and 9% for kittens. These percentages may not be exact since I’m sure some samples were positive for more than one type of parasite, but they give us a ball park figure.
However, a couple of issues suggest that these estimates are actually too low. First of all, whipworms are notoriously hard to diagnose via fecal exam. Their eggs don’t float very well in the most commonly used type of solution, and the worms release their eggs on an intermittent basis (in other words, the worms are present but their eggs are not). Secondly, while hookworms, roundworms, tapeworms, and whipworms are the “Big Four,” these tables say nothing about the incidence of Giardia, coccidia, and other types of intestinal parasites that can affect dogs and cats. The incidence of parasitism in pets is probably significantly higher than what the Banfield numbers show. In fact, a study published in 2009 looking at over a million canine fecal samples submitted to Antech Diagnostics revealed that 29.6% of those coming from dogs less than six months of age and were positive for intestinal parasites. Wow! So next time you head to the veterinary clinic, make sure you bring along a sample of your pet’s poop. You might be surprised at what’s hiding inside. DOES YOUR DOG REALLY NEED LAMB, BISON, AND OTHER 'HYPOALLERGENIC' DOG FOOD PROTEINS?
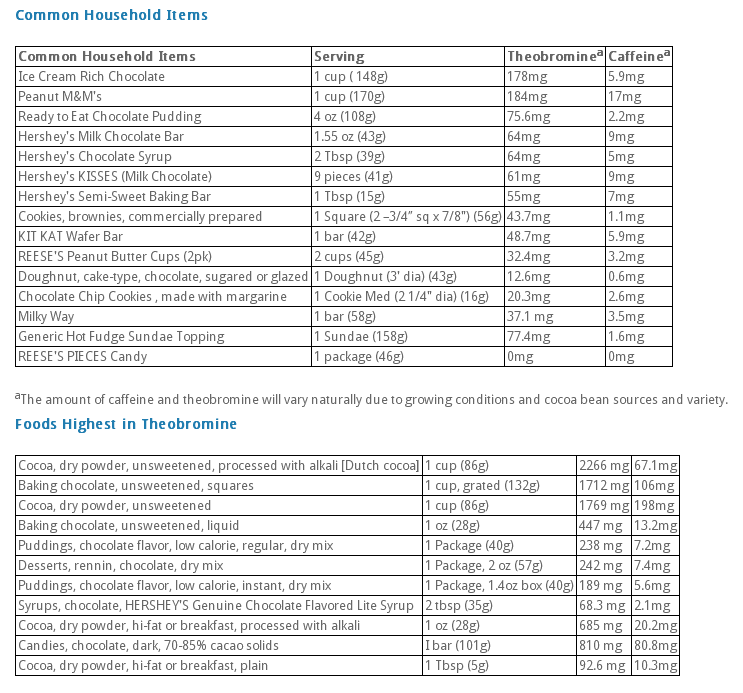
In order to identify what is the best food for dogs with food allergies you must first understand what are food allergies and what causes them. Many different terms are used to describe abnormal reactions to food. The terms “allergy” and “hypersensitivity” describe an immunologic reaction to food allergens and requires previous exposure to the allergen to bring about symptoms. In contrast, a food “intolerance” does not involve the immune system and can occur with the first exposure to a certain food. Both reactions produce similar symptoms and may be difficult to tell apart without veterinary guidance. In fact, according to Dr. Adam Patterson, clinical assistant professor and Chief of Dermatology at the Texas A&M College of Veterinary Medicine & Biomedical Sciences Small Animal Clinic, “Food allergies in dogs present themselves quite differently than food allergies in humans. For instance, a person who is allergic to shellfish may experience throat swelling and possibly a critical or fatal reaction, but in dogs, the allergy is expressed through the skin and seen most often as itch.” WHAT ARE THE COMMON SIGNS OF FOOD ALLERGIES IN DOGS? Symptoms of food allergies in dogs vary, but the most common complaint is non-seasonal itching that may involve the whole body or be focused on the ears and feet. Chronic or recurrent ear and skin infections are also typical. Some dogs may even develop vomiting, diarrhea, or excessive gassiness. Symptoms often begin when dogs are young (before one year of age), but may develop at any time. WHAT CAUSES FOOD ALLERGIES IN DOGS? Dogs with food allergies are typically allergic to proteins, which come from animal or plant-based ingredients of the diet. The proteins are broken down into molecules that the immune system misidentifies as a potential threat. Beef, dairy, wheat, and chicken are the most common culprits of food allergies in dogs. The development of food allergies, however, takes time. So the dog may have been eating the offending ingredients for quite a long time before symptoms develop. HOW IS A FOOD ALLERGY DIAGNOSED IN DOGS? A food trial using a “hypoallergenic” dog food is the only reliable way to diagnose food allergies in dogs. There are two ways to do this – using a novel protein source or hydrolyzed protein. A “novel” protein source is one that is completely new to the dog, thereby reducing the chance of an immune response. In addition, the diet should contain a novel, single source of carbohydrates since plants also contain protein. Hypoallergenic dog food options include venison and potato, duck and pea, salmon and potato or even kangaroo, as long as the dog hasn’t been exposed to these ingredients in the past. Lamb used to be considered hypoallergenic but is now in so many commercial dog foods that it is no longer novel. Hydrolyzed diets are made when intact animal proteins are broken down into very small molecules that the immune system should not be able to recognize as allergens, virtually eliminating the possibility of an adverse food reaction. Starch or rice are typically used as carbohydrate sources because they are very infrequently associated with allergic reactions. Whatever type of hypoallergenic dog food is used, it should be fed for a minimum of 8-10 weeks to adequately assess the dog’s response. Most dogs experience at least a partial improvement in their food allergy symptoms within the first 4-6 weeks, but several dog breeds (including Labrador Retrievers and Cocker Spaniels) may require a longer period of time to respond. It is important to feed only the hypoallergenic dog food, avoiding all other foods, treats and even flavored medications such as chewable heartworm preventives, antibiotics, and pain relievers. Once the food allergy has been diagnosed using a hypoallergenic dog food, a challenge should be performed to confirm the diagnosis. When the original diet is fed, the symptoms should return within two weeks. Following confirmation of the food allergy, single source ingredients (e.g., slices of chicken or a sprinkling of wheat) may be added to the hypoallergenic dog food to determine exactly which ingredients must be avoided in the future. WHAT IS THE BEST FOOD FOR DOGS WITH ALLERGIES? It is important to work with a veterinarian to determine the best food for dogs with allergies. Novel protein and hydrolyzed diets that are available by prescription only are superior to those that can be bought over the counter because the latter often contain trace amounts (or more) of common allergens, even if they are not listed on the label. Randomly eliminating ingredients from your dog's diet without the input of a veterinary nutritionist is also a bad idea, as it can result in nutritional imbalances and is unlikely to identify the underlying problem. Save yourself the worry and speak with your veterinarian if you suspect that your dog has a food allergy. References Patterson, A. Itchy Dogs: Is Food the Problem? Texas A&M University, Veterinary Medicine and Biomedical Sciences. Accessed February 3, 2014. Thomas, R.C. Food Allergy in Dogs & Cats. Presented at the 2005 Western Veterinary Conference, Las Vegas, NV. What Makes Chocolate Toxic to Dogs Chocolate contains substances known as methylxanthines (specifically caffeine and theobromine), which dogs are far more sensitive to than people. Different types of chocolate contain varying amounts of methylxanthines. In general, though, the darker and more bitter the chocolate the greater the danger. For instance, 8 ounces (a ½ pound) of milk chocolate may sicken a 50-pound dog, whereas a dog of the same size can be poisoned by as little as 1 ounce of Baker's chocolate! Why Isn't Chocolate Toxic to Humans? Humans can break down and excrete methylxanthines such as theobromine much more efficiently than dogs. What Should I Do if My Dog Ate Chocolate? If you know your dog has ingested chocolate , or has any of the symptoms below, contact the Pet Poison Helpline at 1-855-213-6680 or your veterinarian right away. Remember, with any poisoning, it’s always cheaper, less invasive, and has a better prognosis/outcome if you treat early. Once your dog has already developed clinical signs and is affected by the poison, it makes for a much more expensive veterinary visit! Symptoms of concern include:
The association between Ebola and dogs has been all over the news lately. After potentially being exposed by their infected owners, a Spanish dog, Excalibur, was euthanized, while a Texas dog, Bentley, is being held in isolation at an undisclosed location. The disparate handling of these two cases raises the question — what risk do dogs really pose when it comes to the transmission of the Ebola virus?
We do know that Ebola has the ability to infect certain types of animals in addition to humans. Antibodies to the virus are widespread in African fruit bats. Many scientists think that fruit bats may be the natural hosts for Ebola since they do not appear to become sick from the virus, but they do shed it. Nonhuman primates react like people when infected with Ebola, becoming very sick and often dying. Forest antelope can also become infected. Researchers noted that during an Ebola outbreak in Gabon in 2001-2002, “unexplained deaths of animals had been mentioned in the nearby forests” and “samples taken from their carcasses [primates and antelopes] confirmed a concomitant animal epidemic.” Pigs can become infected with the “Reston” variant of Ebola, but this strain does not make people sick. Contact with fruit bats and/or wild animals hunted for food are the most likely initial sources of infection in human Ebola outbreaks. Ebola is a zoonotic disease (a disease that can be transmitted from animals to people) even though by far the most common route of transmission once an outbreak has started is person to person. All of this means that concerns about dogs living in close contact with Ebola victims are not unreasonable. In fact, research looking at the Gabon outbreak showed that approximately 25 percent of the dogs in the region had produced antibodies against the Ebola, indicating they had been exposed to the virus. This does not mean, however, that the dogs actually “had” Ebola or could transmit it to people or other animals. As the Centers for Disease Control says on its website, “At this time, there have been no reports of dogs or cats becoming sick with Ebola or of being able to spread Ebola to people or animals.” A few weeks ago, I spoke to Dr. Ronald Harty, associate professor of microbiology at Penn Vet, about his research into a potential drug to combat Ebola. I think he explains the situation best. As quoted in Delaware Online, The News Journal: “The dog's immune system reacted to the virus it came in contact with but did not replicate it," Harty said. That means the dog's body recognizes there was a threat present and created antibodies to fight it, but the virus didn't create more copies of itself and spread, as a viral infection does. "It is highly unlikely a dog, cat or any other domestic animal could contract or transmit the disease.” Because of this extremely low chance of disease transmission, the World Small Animal Veterinary Association recommends that, in cases like Excalibur’s and Bentley’s, dogs be quarantined and tested but not immediately euthanized. Kudos to the authorities in Dallas who let science rather than unfounded fear guide their decision making. Article By Dr. Coates References Ebola virus antibody prevalence in dogs and human risk. Allela L, Boury O, Pouillot R, Délicat A, Yaba P, Kumulungui B, Rouquet P, Gonzalez JP, Leroy EM. Emerg Infect Dis. 2005 Mar;11(3):385-90. Reston ebolavirus in humans and animals in the Philippines: a review. Miranda ME, Miranda NL. J Infect Dis. 2011 Nov;204 Suppl 3:S757-60. [Multiple Ebola virus haemorrhagic fever outbreaks in Gabon, from October 2001 to April 2002]. Nkoghe D, Formenty P, Leroy EM, Nnegue S, Edou SY, Ba JI, Allarangar Y, Cabore J, Bachy C, Andraghetti R, de Benoist AC, Galanis E, Rose A, Bausch D, Reynolds M, Rollin P, Choueibou C, Shongo R, Gergonne B, Koné LM, Yada A, Roth C, Mve MT. Bull Soc Pathol Exot. 2005 Sep;98(3):224-9. French. |
The PAW Blog...
For the LOVE of Pets The goal of this blog is to help educate pet owners by sharing pet health facts and pet news articles...and ... sometimes put a smile on your face with a cute or funny pet story! Categories
All
Archives
April 2024
Search for any topic...
|

 RSS Feed
RSS Feed

